I. Overview of Asthma
Definition
Asthma is a chronic lung disease characterized by the narrowing and swelling of airways, often accompanied by the production of excess mucus. These changes can make breathing difficult and trigger coughing, wheezing, and shortness of breath. Asthma requires ongoing medical management and can become life-threatening if not properly treated.
Prevalence
Asthma affects over 25 million individuals in the United States, including more than 5 million children. This widespread condition impacts people of all ages and can significantly interfere with daily activities if not effectively controlled.
II. Symptoms and Signs
Common Symptoms
Asthma presents with a variety of symptoms that can vary in intensity. Common symptoms include shortness of breath, chest tightness, pain, or pressure, and wheezing, which is particularly noticeable during exhalation. Many individuals with asthma also experience coughing, especially at night, and difficulty sleeping due to these respiratory issues.
Worsening Signs
Signs that asthma may be worsening include an increased frequency and severity of symptoms. Individuals may find themselves relying more heavily on quick-relief inhalers to manage their condition. These indicators suggest that asthma is not well-controlled and that medical intervention may be necessary to adjust treatment plans.
III. Types of Asthma
Intermittent Asthma
Intermittent asthma is characterized by symptoms that come and go. Individuals with this type of asthma typically experience periods of normal breathing between asthma flares.
Persistent Asthma
Persistent asthma involves continuous symptoms, which are categorized by their severity into mild, moderate, or severe. This type requires ongoing management to keep symptoms under control.
Specific Types
- Allergic Asthma: This type is triggered by allergens such as molds, pollens, and pet dander. It is often associated with other allergic conditions.
- Non-allergic Asthma: Triggered by factors such as exercise, stress, or illness, non-allergic asthma does not involve an allergic reaction.
- Exercise-induced Asthma: Symptoms are triggered by physical activity. This type is also known as exercise-induced bronchospasm.
- Occupational Asthma: This type occurs due to exposure to irritants in the workplace, such as chemicals, dust, or fumes.
- Asthma-COPD Overlap Syndrome (ACOS): This condition involves characteristics of both asthma and chronic obstructive pulmonary disease (COPD), making it particularly challenging to manage.
- Adult-onset Asthma: Asthma that develops after the age of 18. It can be triggered by various factors and often requires different management strategies compared to childhood asthma.
- Pediatric Asthma: This type begins in childhood and can occur in infants and toddlers. While some children may outgrow asthma, others continue to experience symptoms into adulthood. It is important to work with a healthcare provider to manage this condition effectively.
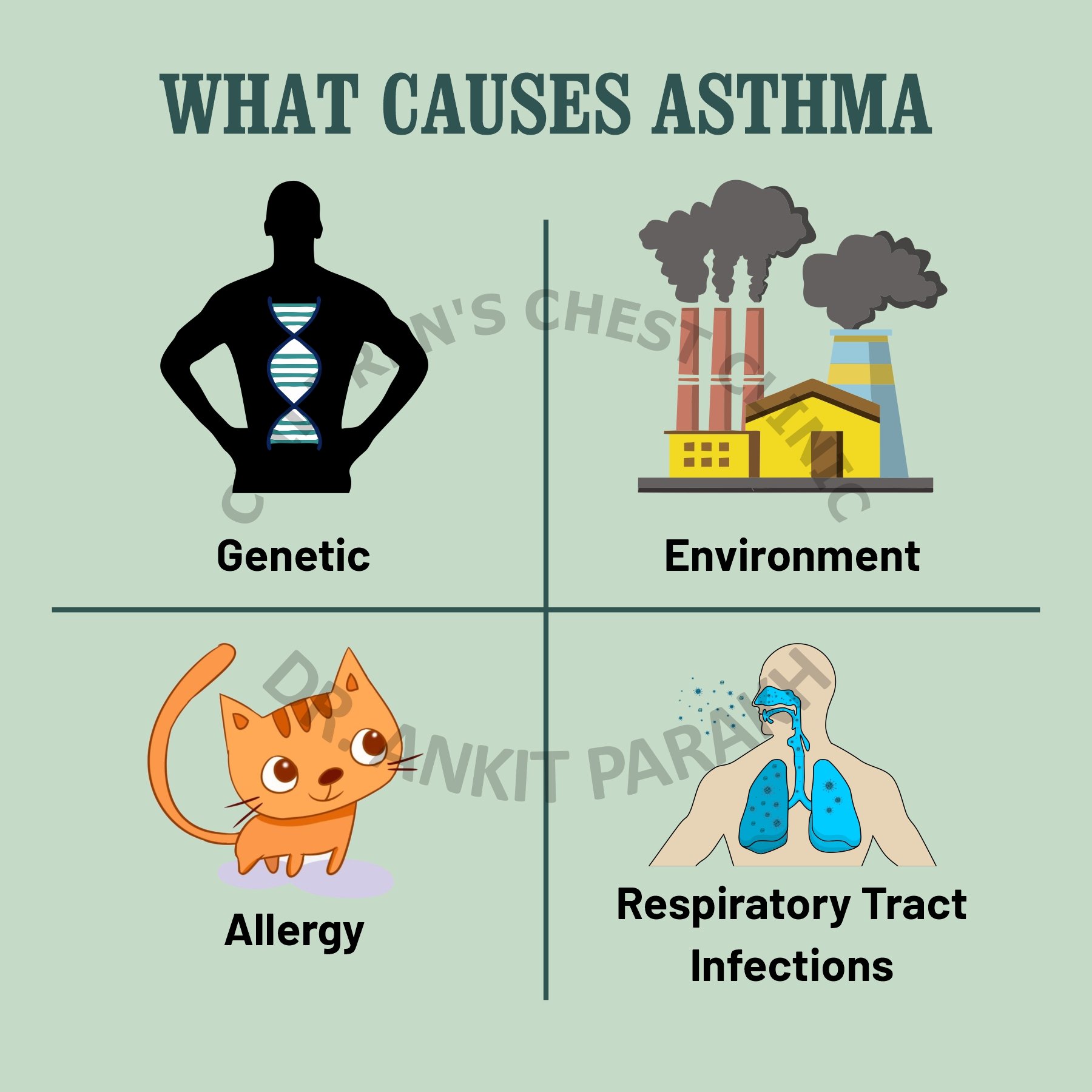
IV. Causes of Asthma
Unclear Exact Causes
The specific cause of asthma remains unknown. It is characterized by inflamed and sensitive airways, which react to various triggers.
Suggested Factors
- Genetics: A family history of asthma or related atopic conditions increases the likelihood of developing asthma.
- Environmental Factors:
- Exposure to allergens such as pollen, dust mites, mold, and pet dander can trigger asthma symptoms.
- Air pollution, including factory emissions, car exhaust, and smoke, is linked to asthma development.
- Lifestyle Factors:
- Smoking and exposure to tobacco smoke, including secondhand and thirdhand smoke, significantly increase asthma risk.
- Obesity is associated with increased inflammation and a higher risk of asthma.
- Premature birth or having a low birth weight can contribute to the development of asthma.
- Infections:
- Respiratory infections during childhood, such as respiratory syncytial virus (RSV) and bronchiolitis, are linked to the later development of asthma.
V. Asthma Triggers
Environmental Triggers
- Airborne Allergens: Common allergens include pollen, dust mites, mold spores, and pet dander. These can provoke asthma symptoms in sensitive individuals.
- Air Pollutants: Smoke, fumes, and ozone are significant environmental pollutants that can exacerbate asthma symptoms.
- Weather Conditions: Sudden changes in temperature, cold air, wind, thunderstorms, heat, and humidity can all trigger asthma attacks.
Lifestyle and Emotional Triggers
- Physical Activity and Exercise: Vigorous physical activity can induce asthma symptoms, especially if not managed properly.
- Strong Emotions and Stress: Emotional responses such as stress, anxiety, or excitement can lead to asthma flare-ups.
- Laughter: Intense laughter can also trigger asthma symptoms in some individuals.
Medical Triggers
- Medications: Certain medications, including beta blockers, aspirin, and nonsteroidal anti-inflammatory drugs (NSAIDs), can provoke asthma symptoms.
Other Triggers
- Infections: Respiratory infections such as colds, flu, and COVID-19 can worsen asthma symptoms.
- Mould or Damp Environments: Exposure to mould or damp conditions can trigger asthma.
- Poor Air Quality: Areas with poor air quality can exacerbate asthma, making it crucial to monitor and manage exposure to polluted environments.
VI. Risk Factors
Genetic Predisposition
A family history of asthma or related atopic conditions, such as eczema, hay fever, or food allergies, significantly increases the likelihood of developing asthma.
Atopic Conditions
Individuals with atopic conditions, including eczema, hay fever, and food allergies, are at a higher risk of developing asthma.
Lifestyle Factors
- Smoking and Exposure to Tobacco Smoke: Both active smoking and exposure to secondhand smoke are major risk factors for asthma.
- Obesity: Excess body weight is linked to increased inflammation and a higher risk of asthma.
- Premature Birth or Low Birth Weight: Being born prematurely or with a low birth weight is associated with a greater risk of developing asthma.
Occupational Exposure
Exposure to certain chemicals, dusts, and fumes in the workplace can increase the risk of developing asthma. This is particularly relevant for individuals in industries such as manufacturing, farming, and hairdressing.
Demographic Factors
- Gender: Asthma is more prevalent in boys during childhood and more common in women during adulthood.
- Race and Ethnicity: Higher prevalence rates of asthma are observed in Puerto Rican, Black, and African American populations, indicating a need for targeted awareness and intervention efforts in these communities.
VII. Diagnosis and Tests
Medical History
A thorough review of your medical history is crucial for diagnosing asthma. This includes personal and family history, focusing on any occurrences of allergies, eczema, and lung diseases. Understanding these factors helps healthcare providers determine the likelihood of asthma and related conditions.
Spirometry
Spirometry is a key diagnostic tool used to measure airflow. It assesses how much air you can exhale after a deep breath and how quickly you can do so. This test helps in diagnosing asthma and monitoring its progression and response to treatment.
Additional Tests
- Chest X-ray: A chest X-ray can help rule out other conditions that might mimic asthma symptoms.
- Blood Test: Blood tests can identify the presence of allergens and assess overall health, aiding in the diagnosis of asthma.
- Skin Test: Skin tests can determine specific allergic triggers that may be contributing to asthma symptoms. This information is vital for creating an effective management plan.
VIII. Management and Treatment
Medications
- Bronchodilators: These medications relax the muscles around the airways, making it easier for air to flow through. They are essential for providing quick relief from asthma symptoms.
- Anti-inflammatory Medicines: These drugs help reduce swelling and mucus production in the airways, making it easier to breathe. They are typically used for long-term control of asthma.
- Biologic Therapies: These treatments are used for severe asthma cases that do not respond to standard medications. They target specific molecules in the immune system to reduce inflammation and prevent asthma attacks.
Administration Methods
Asthma medications can be administered in various ways to ensure effectiveness and convenience:
- Inhalers: Metered-dose inhalers and nebulizers deliver medication directly to the lungs for quick and efficient relief.
- Oral Medications: These include pills and liquids taken by mouth, often used for long-term control.
Asthma Control Goals
Effective asthma management aims to:
- Maintain Normal Activities: Allow individuals to engage in everyday activities without restriction.
- Minimize Symptoms: Reduce the frequency and severity of asthma symptoms to improve quality of life.
- Reduce Reliance on Rescue Inhalers: Limit the need for quick-relief inhalers, indicating better overall asthma control.
- Ensure Uninterrupted Sleep: Prevent nighttime symptoms that can disrupt sleep, promoting overall health and well-being.
IX. Prevention and Monitoring
Identify and Avoid Triggers
Identifying and avoiding asthma triggers is crucial for managing symptoms effectively. Common triggers include allergens, air pollutants, certain foods, and stress. By recognizing these triggers, individuals can take proactive steps to minimize exposure and prevent asthma flare-ups.
Healthy Lifestyle
Maintaining a healthy lifestyle plays a significant role in asthma management. This includes keeping a clean environment to reduce exposure to allergens like dust mites and mold. A balanced diet rich in fruits, vegetables, and whole grains supports overall health and can help reduce inflammation associated with asthma.
Monitoring Tools
Using monitoring tools such as peak flow meters helps in tracking lung function. These devices measure how hard and fast you can exhale, providing valuable information about your airway status. Regular monitoring allows for timely adjustments to treatment plans, ensuring optimal asthma control and reducing the risk of severe attacks.
X. Emergency Management
Severe Asthma Attack
In the event of a severe asthma attack, it is crucial to use a rescue inhaler immediately. This quick-relief medication helps to open the airways and make breathing easier. If symptoms do not improve rapidly after using the inhaler, or if breathing difficulties are severe, seek medical help immediately. Prompt action is essential to prevent potentially life-threatening complications.
Asthma Action Plan
An asthma action plan is a personalized guide developed with your healthcare provider. It outlines the steps to take in managing asthma daily and during an attack. The plan includes information on:
- Recognizing early signs of an asthma attack.
- Using medications correctly and at the right times.
- Knowing when to escalate treatment.
Understanding when to seek emergency care.
- Having a clear action plan helps manage symptoms effectively and reduces the risk of severe asthma episodes.
XI. Living with Asthma
Prognosis
With proper management, individuals with asthma can lead productive lives and participate in various activities. Effective treatment plans and regular monitoring allow for the control of symptoms, enabling individuals to maintain a high quality of life.
Nighttime Asthma
Nighttime asthma, also known as nocturnal asthma, can significantly impact sleep quality. To address this, it is important to identify and mitigate triggers in the bedroom, such as dust mites and pet dander. Adjusting sleeping positions and ensuring good control of daytime symptoms can also help reduce nighttime flare-ups.
COVID-19 Considerations
Individuals with asthma may be at a higher risk for severe outcomes if they contract COVID-19. It is crucial to stay informed about the importance of vaccination and to follow public health guidelines to avoid exposure. Regular communication with healthcare providers can ensure that asthma management plans are adjusted to address any additional risks posed by COVID-19.
Additional Notes
Occupational Asthma
Occupational asthma is a form of asthma triggered by exposure to substances in the workplace. It is important to recognize and manage this type of asthma to prevent long-term health issues.
- Common Triggers:
- Isocyanates
- Flour and grain dust
- Colophony (found in solder fumes)
- Latex
- Animal exposure
- Wood dust
- High-Risk Professions:
- Paint sprayers
- Bakers
- Pastry makers
- Nurses
- Chemical workers
- Animal handlers
- Timber workers
- Welders
- Food processing workers
Identifying and mitigating exposure to these triggers can help manage occupational asthma effectively and protect the health of individuals in these professions.